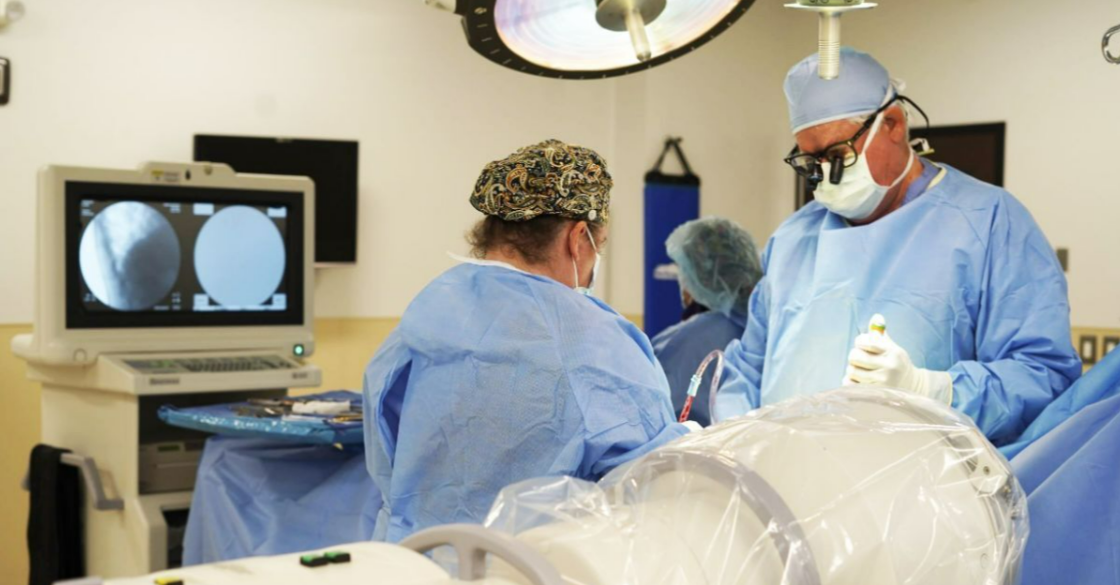
For many patients, the day of spine surgery feels like the finish line. The reality for most, though, is that it’s just one part of a much longer journey. Dr. Larry Davidson, a leader in minimally invasive spine surgery, reminds patients that success after surgery depends heavily on what happens during recovery, especially through targeted physical therapy.
While surgical techniques continue to improve, outcomes are not defined solely by what happens in the operating room. Rehabilitation plays a pivotal role in protecting surgical gains, rebuilding strength and helping the spine return to function in the months and years that follow. Spine health is dynamic, and post-operative care must be, too.
Why Surgery Alone Isn’t Enough
Spinal procedures may relieve pressure on nerves, correct deformities or stabilize unstable segments, but they don’t fix dysfunctional movement or rebuild weakened muscles. In many cases, those problems contributed to the issue in the first place.
Without focused rehab, patients risk developing compensatory habits, muscle imbalances or lingering inflammation that can undermine surgical outcomes. They may also miss the opportunity to recondition muscles and joints that were limited prior to surgery. Physical therapy helps close this gap. It’s not just about managing pain. It’s about retraining the body to move better, so future injuries are less likely to occur.
Relearning Movement in a Healing Body
Post-surgical tissues need time to repair, but they also need guidance. Movement patterns must adapt around healing incisions, surgical hardware and soft tissue changes. Physical therapists begin by teaching patients how to move safely, get in and out of bed, walk upright and protect the spine during daily activities. These early strategies reduce stress on healing tissues and improve confidence.
Gradually, therapy introduces range-of-motion exercises, strength-building drills and neuromuscular retraining. Patients relearn how to sit, stand, lift and walk using better form, supported by stronger muscle engagement and improved balance. These lessons shape how the spine functions by moving forward.
Preventing Regression and Setbacks
Recovery isn’t always linear. Without consistent guidance, it’s easy to fall back into pre-surgery habits that can trigger discomfort or dysfunction. Rehabilitation helps patients avoid common pitfalls such as:
- Favoring one side due to surgical discomfort
- Avoiding certain movements out of fear
- Using poor form while lifting, walking or sitting
These behaviors can place excess strain on healing areas or stress surrounding joints. Therapy ensures patients build strength symmetrically, maintain alignment and restore proper biomechanics as they resume everyday tasks. With support, setbacks can often be identified early and corrected before they become serious issues.
Supporting Long-Term Spinal Health
Surgical success isn’t measured by pain relief alone. It’s also about returning to work, recreation and family life, without restrictions or dependence on medication. Physical therapy supports this return by:
- Improving muscular endurance
- Enhancing joint mobility
- Reinforcing core stability
- Teaching self-management skills
Dr. Larry Davidson notes that patients who complete physical therapy tend to report higher satisfaction, lower re-injury rates and greater function than those who stop therapy early or skip it altogether. Rehab is about sustainability. It gives patients the tools they need to protect their spine long after the surgical wound has healed.
Building Independence Through Education
Therapists do more than supervise exercises. They educate patients about body mechanics, ergonomics, pacing and warning signs of overuse. These lessons are vital for maintaining progress outside the clinic.
For example, patients learn how to modify workstations, adjust sleep positions, or avoid repetitive stress during their hobbies. They practice safe ways to lift children, carry groceries or garden, without risking setbacks. Education turns therapy into a long-term strategy, not just a short-term fix.
When Recovery Becomes Performance
Some patients return to high levels of activity after spine surgery, including sports or physically demanding jobs. In these cases, physical therapy bridges the gap between basic mobility and peak performance.
Advanced rehabilitation may include agility drills, strength training or sport-specific exercises tailored to everyone’s goals. Functional tests assess readiness, symmetry and endurance to ensure the spine is fully prepared for real-world demands. Rehab doesn’t stop at being “pain-free.” It continues until the patient is confident, capable and fully reconditioned.
Addressing the Psychological Side of Recovery
Surgery can be mentally taxing. Patients often face fear of re-injury, frustration with limitations or anxiety about their future health. These emotional factors influence motivation and movement patterns.
Physical therapists provide reassurance, structure and encouragement during this uncertain time. They help patients focus on what they can do, rather than what they can’t, building momentum one small milestone at a time. This mindset is critical. Recovery is as much psychological as it is physical, and therapy supports both sides of that equation.
Tailoring Therapy to the Procedure
Different spinal surgeries call for different rehab plans. A lumbar fusion requires a different approach than a cervical discectomy or scoliosis correction.
Therapists work closely with surgeons to understand the specific procedure, any precautions or restrictions and the patient’s pre-op condition. This collaboration helps ensure the plan supports healing, without jeopardizing surgical integrity. For example:
- Fusion patients may avoid twisting or bending early on
- Disc patients may focus on core activation to support the spine
- Decompression patients often benefit from neural mobility drills
Customized therapy respects the healing timeline, while pushing toward the best possible result.
The Role of Consistency and Timing
Starting therapy too soon or too late can impact recovery. Early movement must be gentle and strategic. Waiting too long can allow stiffness and weakness to set in.
Surgeons typically provide a rehab timeline, but the most important factor is consistency. Attending scheduled sessions, completing home exercises and gradually progressing helps build a stable foundation. Recovery doesn’t happen in a week. But with steady effort, each session builds on the last.
Making the Most of the Process
Patients who view physical therapy as an extension of their surgery, not a separate event, tend to fare better. They understand that healing doesn’t end with sutures. It ends when movement is restored, pain is reduced and life feels full again.
Therapy isn’t just a phase, but it’s a key part of the outcome. It reinforces the progress made during surgery and helps prevent setbacks that could delay healing. By staying engaged in therapy, patients rebuild strength, restore confidence and reclaim their independence.
From Recovery to Resilience
Beyond the incision lies the opportunity to regain strength, mobility and confidence. Physical therapy gives patients the tools to protect their spines, prevent future injuries and move freely again.
It also empowers them to take an active role in their recovery, something no procedure alone can guarantee.
Spine surgery may start the process, but therapy carries it forward. In that partnership, long-term success is not only possible, but it’s expected to be successful. Each session builds on the foundation set in the operating room, translating surgical precision into real-world progress. When patients commit to both, the journey toward lasting relief and restored function becomes a shared, achievable goal.